During the COVID-19 pandemic, there were worldwide shortages of personal protective equipment (PPE), especially surgical N95 respirators and masks, including many hospitals in Thailand. The Thoracic Society of Thailand and US. Centers for Disease Control and Prevention suggested acceptable alternative personal protective equipment with respect to surgical masks or industrial N95 respirators.1,2 In general, a surgical mask protects healthcare workers against large droplets. An N95 respirator reduces healthcare worker exposure to particles including aerosols and large droplets. However, surgical masks or N95 equivalent ear-loop masks are a loose-fitting type, which in turn cause leakage around the edge of the mask when the user inhales. On the other hand, N95 respirators are tight-fitting which requires a seal check each time the respirator is worn.3
Selection of an appropriate respirator is the first step of Respiratory Protection Program. Other components are training, fit testing, inspection, cleaning, maintenance, storage, evaluation, work area surveillance, and air quality improvement.4 The most critical aspect of respirator use is insufficient fitting. Many healthcare workers think that a seal check is a fit test, which is wrong. A quantitative method is required for better assessment of proper use of respirators.5
According to the Department of Disease Control, Ministry of Public Health Thailand on April 8, 2020, there were 55 healthcare workers who had work-related COVID-19 disease.6 Our study investigated the fit factor by QNFT PortaCount to find acceptable alternative facemasks or respirators when caring for patients with confirmed or suspected COVID-19 in order to protect healthcare workers from work-related COVID-19 disease in Thailand.
A total of 31 quantitative fit tests were performed by two testers, male and female, on various types of masks and respirators using PortaCount Model 8048, TSI Incorporated, Minnesota, USA, following OSHA modified ambient aerosol condensation nuclei counter (CNC) quantitative fit testingprotocols.7 The first tester was a slender woman, 157 centimeters in height and 47 kilograms in weight. The second tester was a moderate size man, 175 centimeters in height and 80 kilograms in weight. Both testers were reviewed with OSHA respirator medical evaluation questionnaires before the study was performed.8,9
Testers followed the modified ambient aerosol CNC protocol for filtering face piece respirators described in Table 1. Testing environment is shown in Figure 1. To assess the effects of sealing, quantitative fit factors were compared between unsealed and sealed surgical masks, selected N95 masks and respirators. Sealing was done using 1 inch 3M micropore surgical tape around the rim of tested masks or respirators.
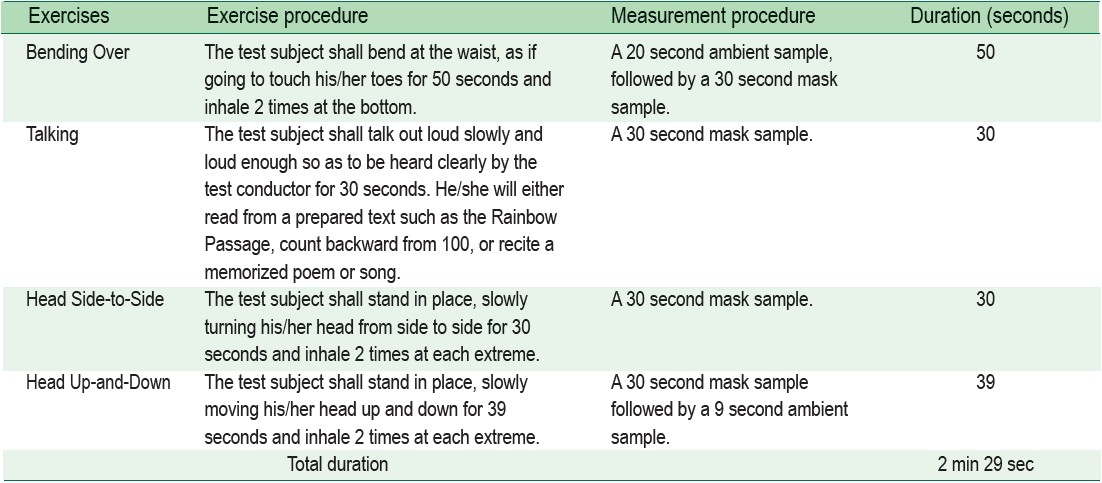
Table 1: OSHA Modified ambient aerosol CNC quantitative fit testing (PortaCount) protocol for filtering face piece respirators.8
The study team selected masks and respirators according to availability, in particular those currently being used in clinical practice. Selected mask and respirators under testing were.
3M Surgical mask
Venus N95 V4400 respirator
3M R95 8247 respirator
3M N95 Vflex 9105 respirator
NASK Nanofiber Smart Mask
Koken Hi-luck 350 N95 respirator
3M surgical N95 1870+ respirator
An online purchased KN95 mask
Putting together test results, it appeared that sealing a surgical mask with one-inch micropore improved performance by seven to eight times, from 4 to 33 by tester 1 and from 5 to 38 by tester 2. Sealing also had profound effects on performance of N95 respirators. The study team found it difficult to seal cup-shaped N95 respirators because of the solid frame. Sealing these respirators had less effect than body size (and face size) of testers. Cup-shaped N95 under testing fitted tester 2 (moderate size male) better than tester 1 (slender female). One type of standard supplied N95 respirator performed well even when not sealed while another type of online supplied N95 mask did not pass the tests even when it was sealed with one inch micropore.

Figure 1: Tester 1 and testing environment.
Surgical masks are designed to prevent the spreading of droplets from wearers whilst respirators are designed to protect the wearers from a contaminated environment. In the situation of COVID-19 pandemic, the preferred “half face” protective device for healthcare workers caring for suspected or confirmed COVID-19 cases should perform, at least as good as OSHA standard i.e. by a minimum fit factor pass level of at least 100. We report the performance of masks and respirators in our study in Figure 2.
Table 2: Quantitative fit factors by testers and types of masks and respirators
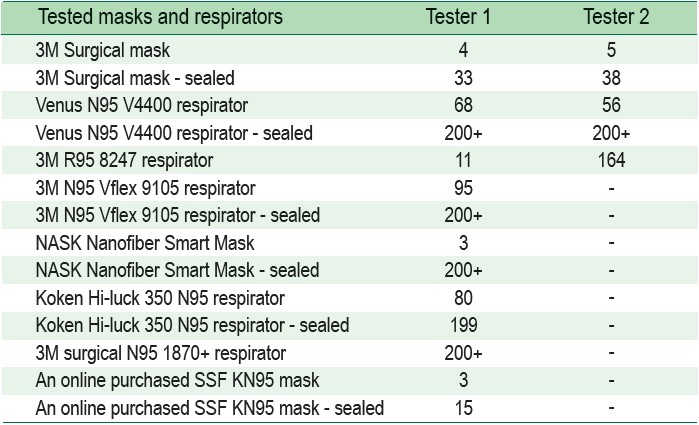
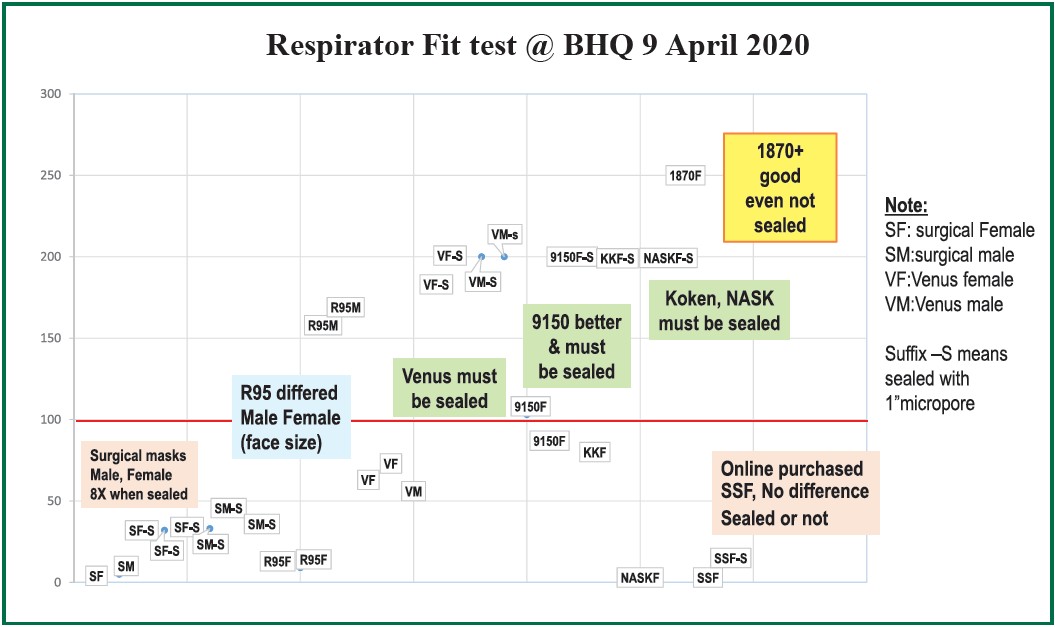
Figure 2: Summarized quantitative fit test results with interpretation
We assessed fit factors of selected masks and respirators that are currently or are candidates for use by healthcare workers caring for patients with confirmed or suspected COVID-19 in a private hospital in Thailand. The results showed that, among N95 respirators, the fold-type respirators passed fit factors without sealing. This could be due to the characteristic of a more freely flexible nosepiece of the fold-type than the cup-type. The cup-type respirators might depend on the face size of testers or sealing to pass the fit test. Therefore, a proper size selection of cup-type respirators should be considered in the first instance.10 The study was conducted when supply of masks and respirators were limited. As a result, only a small number of masks and respirators were available for both tester 1 and 2.
Our assessment complied with US-CDC recommendations to perform fit testing during emerging infectious disease outbreaks because we found significant improvement after sealing tested respirators with one inch micropore tape. In the situation where individual fit testing is not available for every healthcare worker, the practice of “always seal” is recom- mended.
Our findings revealed moderate level of protection of sealed surgical masks (fit factor = 33 - 38). Although significantly increased from non-sealed (fit factor = 4-5), use of surgical masks in high risk situations should be cautioned.
Performance of loose-fitting masks with high quality materials (e.g. N95, FFP2, KN95, KF94 levels) could be improved by sealing. Our findings showed improved fit factor (from 3 to 200+) equivalent to standard N95 respirators. This adaptation should be accompanied with fluid protective device; such as face shields or covering on top with surgical masks as acceptable alternative PPE (personal protective equipment).
With rapid use and high demand for PPE, including surgical masks and respirators, quality control must not be compromised. Regulatory bodies at the national and local level have to ensure inspection of each supply lot particularly when procured online.
Our study primarily revealed fit factors, which represented a ratio of particles between the outside and inside of a mask or respirator. Environmental factors often determine protective outcomes. In high-risk situations such as emergency rooms, intensive care units, or any respiratory aerosol generating procedures, high performance PPE might not be sufficient. Other work place controls, such as engineering, administrative and safe work practices, must be concurrently implemented.11
Sealed surgical mask and sealed NASK nanofiber smart mask could be reliable alternative PPE for healthcare workers during the COVID-19 pandemic. In the situation where PPE supply is limited, we suggest “always seal” available masks and N95 respirators when respirator fit testing could not beperformed. Respirator fit testing as part of respiratory protection program is strongly recommended for better protection of healthcare workers in emerging infectious disease outbreaks.
The authors have no conflict of interest with products, materials or equipment tested and us