The concern for appropriateness of healthcare resources utilization andcost containment have been raised worldwide. Various measures andtools, such as AEP (Appropriateness Evaluation Protocol), ISDcriteria (Intensity of service, Severity of illness, Discharge screens), andapplication of other defined criteria or expert opinion, have been used todetermine admission appropriateness in order to ensure an effective utilizationof hospital beds.1-6 Utilization management (UM) employing those toolstogether with regular informational feedback to hospital management andphysicians are effective in reducing inappropriate admission.7-10 However,those direct measures significantly add administrative burdens to third-partypayers, particularly in performing concurrent management of all inpatienthospitalizations.11-12 Thus, some indirect measures such as admission rates, length-of-stay, and costs benchmarking among hospitals havebeen widely used to induce hospitals and physicians to utilizeresources efficiently.13
The term “simple disease” has been used in health insuranceindustry in Thailand to indicate a group of illnesses that arediagnosed and treated at out-patient departments (OPD) andmostly do not require admission to in-patient departments(IPD). The reason “simple disease” is particularly importantis because both health care providers and insurance partnerswant to avoid misuse of resources. However, this is not alwaysachieved due to complexity of situations where diagnosisrequires some laboratory results or duration of observation.Sometimes, cases that look simple at the beginning turn outnot to be so simple after thorough clinical assessments. Withfast processing of paper work, final diagnoses sometimes werenot appropriately determined. In these cases, disagreementbetween health care providers and payers happens and thuscomplicating approval for reimbursement. With limitedamount of human resources to perform thorough audits,medical experts of third party (insurance) partners thusformulate lists of simple diseases to screen out reimbursementof in-patient department expenses. These lists usually containcommon medical conditions such as upper respiratory tractinfection, pharyngitis, gastritis, gastroenteritis, headache andvertigo. However, once a complication is detected, physiciansin charge may often decide to keep patients in for moreinvestigation and care.
Despite the fact that medical necessity and appropriatenessof care can be evaluated using existing evidence-based criteriaor clinical guidelines, inappropriate admission may beinfluenced by many other potential factors, including patientpreferences, convenient access to hospital, cautiousness ofdoctors, geographical environment, and the design ofreimbursement and payment policies etc.14-16
There has been increasing trends of cases with disagreement,and solving this would result in a healthier relationship betweenhealth care providers and third party payers.
A microeconomic theory of moral hazard effect has beenwell described to explain both patient and physician behaviorchange in response to insurance.17-20 Decreasing self-protection anddemanding more healthcare, ex ante- and ex post-, are twotypes of demand-side moral hazard. Supplier-induced demandarising from informational asymmetry between physicians andpatients is also influential in overutilization of resources,especially in the fee-for-service system.20 The impact ofmoral hazard in private health insurance industry in Thailandis intensified through some insurance products providingdaily compensation for each hospitalization day, which iscurrently one of the strongest financial incentives inpatient-induced inappropriate admission.
Strategic planning for the loss-of-interest (Loss) ratio hasbeen implemented by insurance companies to reduce bothdemand side- and supply- side moral hazard, including: (a)concurrent review and retrospective review which is time- andresource-intensive; (b) statistical report review - set targets/thresholds for hospitals which is easier; and (c) cheaper insuranceagents controlled by government or regulatory bodies.
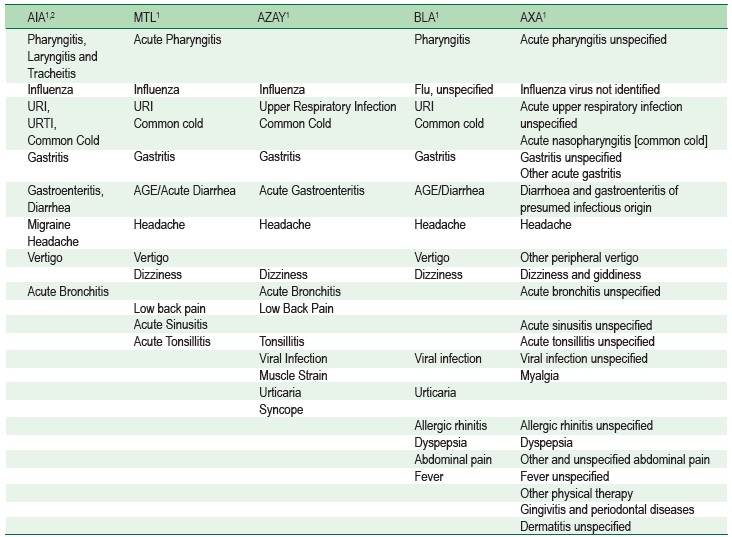
Previous studies have shown patient characteristics andconditions frequently have a high rate of inappropriateadmission.21-23 However, the definition of “simple diseases”has not been well described in any text books or literatures.Most insurance companies in Thailand currently monitor thepercentage of “simple diseases” admission as a key hospitalperformance. Our work here began with the list of existingcases advised by our insurance partners (Table 1). It is clearthat there is a need to develop an objective method to categorizesimple disease from the others primarily to avoid confusionor disagreement. We, therefore, conducted this study toidentify an objective method to guide differentiating complicatedsimple disease cases from non-complicated cases using ThaiDiagnosis Related Groups (DRGs) based on InternationalClassification of Disease (ICD) codes.
In addition to individual case management, another issuethat requires attention is on monitoring of hospitalperformance. With an increasing demand of Thai people totake out insurance coverage to use private instead of publichospitals (Figure 1), competition among insurance salespersonshas resulted in persuasion statements that created expectationsamong enrollees that hospital admissions would be easier withsome insurance plans. The situation creates tensions betweenpatients and physicians with subsequent tensions betweenhospitals and insurance partners. Hospitals with 40 to 50percentages of simple disease admission rates (varied byinsurance partners) were on the spot for being including onthe watch-list. A measure based on comparative analysis is notworthwhile without determining the impacts of different casemix compositions.24 Using one threshold judgment does notprovide any solution to the abuse of resources becauseinsurance enrollees that are able to shop around and tensionswould be even more prevalent. Without an effective solution,this could result in an unhealthy relationship between hospitalsand insurance partners as well. As a result, this studyproposes a more rational method to monitor hospital performanceusing CMI according to level of hospital care.
CMI is an adjusted RW of diagnosis-related groups (DRG)of patients in a health service delivery system (hospital). CMIhas been commonly used as a disease severity index thatreflects mixture of severity among admitted cases. HigherCMI indicates greater proportion of severe cases in a givensetting and duration, and requires more resources and costsfor patient care.26-27 Therefore, CMI can be used to monitorperformance of a health care setting over time. It can also beused to benchmark performance among similar health caresettings. Generally speaking, if a hospital has a high CMI, itis likely that there are more complex than simple cases, andvice versa.
Table 1: List of simple diseases advised by five key insurance partners
Note:
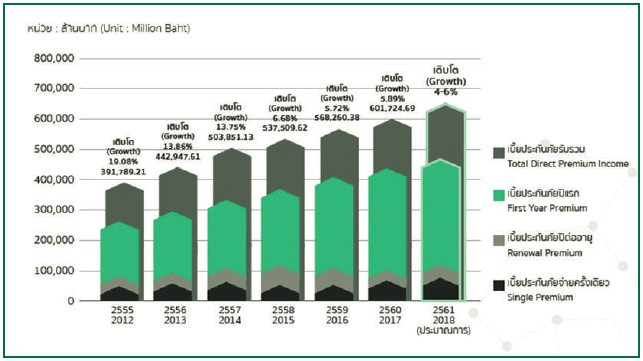
Source: Office of Insurance Commission.
Note: Average growth rates of 9 percent exceed population growth by more than ten times
Figure 1: Increasing trend of insurance coverage in Thailand from 2012 - 2018
A previous study in Thai public hospitals revealed that oneparticular DRG has a different adjusted RW in different levelsof hospitals. For example, adjusted RW for DRG 06570increased from 0.4511 to 0.4607, 0.4620, and 0.5405 inprimary care, secondary care, tertiary care, and teachinghospitals respectively. The result showed that the higherhospital tier, the higher disease severity, even if it is the samediagnosis and same DRG.25
In 2019, BDMS governs 46 hospitals providing healthcarefrom secondary to basic tertiary, hub tertiary and super-tertiarycare levels. Threshold proportion of simple disease admissionof every hospital in the network has been assessed using therange of 40% - 50%. The current level would not allow asecondary care hospital to achieve this target thus having ahigher likelihood of being on the watch-list and this maycomplicate improvement of services. Different thresholds forvarious levels of hospital care (CMI) would, on the contrary,encourage a fine tuning of admissions thus facilitatingdevelopment towards preferred direction of optimum use ofhospital and insurance resources.
This study aims to identify an objective way to labelsimple diseases in order to guide medical practitioners andinsurance partners to utilize resources rationally. Specificobjectives are as follows:
This cross sectional study used three sources of data, i.e.(i) anonymized data from hospital information system, (ii) listof simple diseases recommended by insurance partners, and(iii) selected de-identified claimed records from closed chartreviews supplied by the BDMS Utilization Management andThird Party Payers Services team.
Anonymized data from the hospital information system(HIS) of 34 Hospitals in BDMS in 2017 were used todemonstrate the relationship between CMI and the proportionof Simple Disease admissions. A total of 387,311 cases wereincluded for the calculation of hospital specific CMIs. Hospitalspecific proportion of simple disease cases in 2017 werecalculated based on the list of 31 diseases provided byinsurance partners. These numbers of simple disease casesserved as nominators while the numbers of total admissionsof respective hospitals in 2017 served as denominators. Theprocess resulted in 34 pairs of hospital specific CMIs and theproportion of (theoretical) Simple Disease admissions.
The List of Simple Diseases has been introduced in theBackground section. We first received a list of diagnoseslabeled as “Simple Disease Admission” from one partner.Trying to generalize, we obtained four more lists from keyinsurance partners and summarized them into a list of 31diseases/diagnoses by keeping the same list while adding thedifference. With the concept of RW in mind, we labeled eachdisease/diagnosis with a respective RW and sorted them outto look for the meaningful cut off points to differentiate themajority and mostly agreed upon Simple Diseases. Two cutoff points were identified using interpolation technique. Theseare shown in Table 2 and Figure 3. A total of 1,558 de-identifiedclaimed records in 2017 were then used to represent BDMSUM team viewpoints on Simple Disease perspective. Theywere randomly selected from all claimed records of 33 hospitalsfor internal discussions towards improvement of resourceutilization and accurate medical documentation. Our studyused this dataset to “test” the proposed RW cut off points byshowing different scenarios that would happen, given usingvarious RW cut of points.
Data extraction was in full compliance with Health InsurancePortability and Accountability Act (HIPAA) standards. Datawere analyzed using Statistical Package for Social SciencePersonal Computer (SPSS-PC) version 22 after processingwith online, free access modules of R-Code. Statisticalsignificant difference level was set at 0.05. Data used forthis study will be kept for five years after the date ofpublication.
Relationship between CMI and proportion of simple diseaseadmissions
To assess the nature of health performance of the BDMShospital network, we constructed a scattergram of 34 pairsof hospital specific CMIs and proportion of (theoretical)Simple Disease admissions and found an overall negativerelationship between the two variables, with correlationcoefficient (R) – 0.76, 95% Confidence Interval from -0.59to -0.89, p < 0.01 (Figure 1). To assess whether the relationshipoccurs only among specific groups i.e. claimed admissions,data were stratified and four scatter plots were generated.In addition to Figure 1, the relationship between CMI andproportion of simple disease cases was found to be consistent,among claimed (165,667 cases) and both claimed andunclaimed (total 366,576 cases). Please see Figure 2a, 2b,2c and 2d.
 and proportion.jpg)
Figure 1: Scatter plot between Case Mixed Index (CMI) and proportion of simple diseases among network hospital ofBangkok Dusit Medical Services (BDMS) PLC network hospitals, 2017.
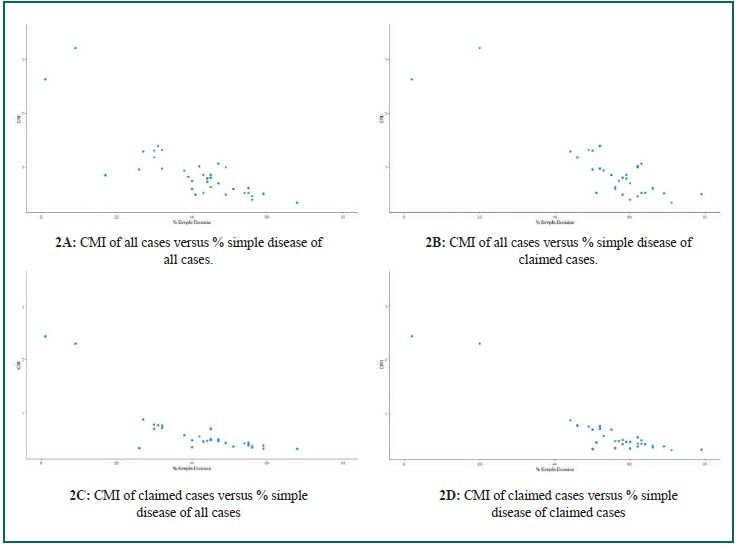
Figure 2: Correlation between CMI levels and proportion of simple disease cases admitted in four scenarios.
Identifying RW cut off points
We mapped the 31 Simple Diseases with their respectiveRWs. With this, we found three clusters of diseases/diagnosis of:
As a result, two cut off points were proposed by interpolatingthe RW of number 22 and 23 (resulting RW equals to 0.3), andinterpolating the RW of number 27 and 28 (resulting RW equalsto 0.4), see Figure 3. The first cut off point of 0.3 would have the power to categorize 22 (71%) of the whole list of 31diseases / outcomes as simple diseases while the other cut offpoint of 0.4 would have the power to categorize 27 (87%) ofthe whole list (Table 2).
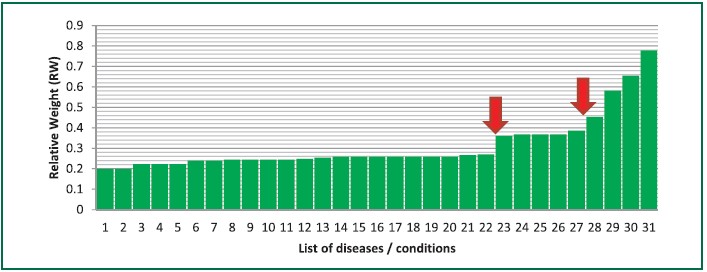
Figure 3: List of the 31 simple diseases by relative weights (RWs)
Different scenarios resulting from using various levels of RWcut-off points

A critical question here is what would happen when weuse different RW cut-off points. The direct effect is that usinga higher RW cut-off point would result in categorizing morecases as “Simple Disease”. We then simulated three scenariosof using 0.3, 0.4 and 0.8 as the cut-off points to the 1,558records of de-identified cases.
Each time a cut-off point was applied to this dataset, itsegregated 1,558 cases into two groups of “more than” and“less than or equal to” the cut-off point. With specific diagnosisfrom this dataset, we brought in data to determine whethereach case was with “complication” or not and labeled themaccordingly. The final step was to label them whether theywere categorized as “Simple Disease” or not. The results ofthree scenarios appear in Figures 4, 5 and 6.
A group of cases requiring attention would be those whichare categorized as simple diseases with complications. Servicedelivery settings and insurance partners share responsibilitieson these potentially complicated cases. In this dataset of 1,558 cases, there are 202 cases with complications, of which 151 cases were categorized as Simple Disease.
In the first scenario of using 0.3 cut-off point, 895 caseswould be categorized as Simple Disease and only 8 amongthem would fall into this potential RM category (Figure 4). For thesecond scenario of using 0.4 cut-off point, 1,143 cases wouldbe categorized as Simple Disease and 44 cases would be inthis potential RM category (Figure 5). Once the threshold of0.8 cut-off point is used, 1,402 cases would be labeled asSimple Disease and number of potential RM cases wouldincrease to 165 (Figure 6). Increasing cut-off point thresholds from 0.3 to 0.4 would increase the number of potential RMcases from 8 to 44 cases (5.5 times) and from 0.4 to 0.8 from44 to 169 cases (3.8 times). It is obvious that while increasingthreshold brings some benefit of detecting more Simple Diseasecases, it also brings along more risks.
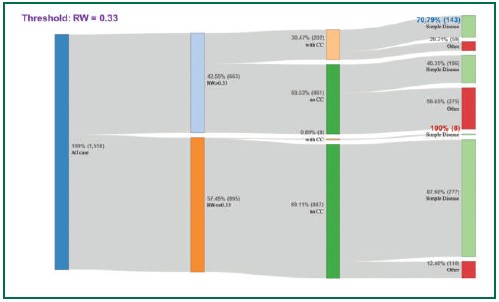
Figure 4: Number of cases categorized into simple or not simple diseases using 0.3 RW cut-off point
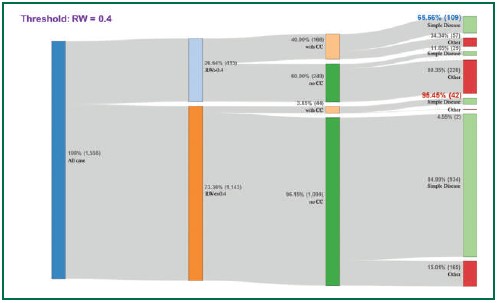
Figure 5: Number of cases categorized into simple or not simple diseases using 0.4 RW cut-off point.
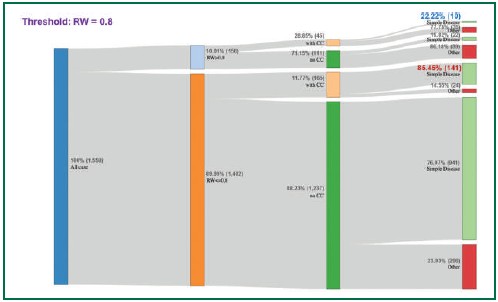
Figure 6: Number of cases categorized into simple or not simple diseases using 0.8 RW cut-off point.
Monitoring hospital performance
Percentages of simple diseases admitted: With differentcomplexity of cases (broad range of CMI among BDMSnetwork hospitals, different levels of percentages of simplediseases should be assigned for the monitoring of hospitalperformance. From 2017, using the total discharged caseswith RW data (n = 366,576), we calculated group specificmedian proportion of simple disease and compared these withmedian proportion of cases below RW = 0.4 and found themto be consistent (Table 3). As a result, an idea of groupspecific “yellow zones” are proposed. The idea follows trafficlights of red, yellow and green that we should have two cut-offpoints of percentages of simple disease cases (identified usingRW – 0.4) admitted. If the average percentage of a hospital isgreater than the upper cut-off point, hospital performance isin the red zone. If the percentage is less than the lower cut-offpoint, the performance is in the green zone. This would givea list of hospitals whose performance is in between two cut-offpoints, i.e. in the yellow zone.
Once hospital performance (reflected by averagepercentages of admission of simple disease identified usingRW = 0.4) stays below these yellow zones, only continuousmonitoring is required. However, when the proportion fallsinto the yellow zones, specific attention should be paid byhospital management. If the situation progresses and theproportion moves to higher than the upper limit of the relevantyellow zone, special interventions of hospital management andinsurance partners will be urgently required.
Although there is no sufficient data currently to determinethe two cut-off points for the construction of the “yellowzones”, we believe it would not be totally incorrect to roundup what we found as group specific median percentages ofcases with RW below 0.4 (Table 3) to define the lower cut-offpoints. The upper ones are more difficult. For the interim, wejust added an absolute amount of 10% to each of the lowerones.
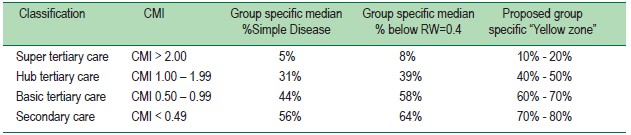
Table 3: Recommended levels of %Simple Disease to be used for various hospital complexity
At the individual-case level, RW 0.4 may be used as ascreening tool for first-level review. However, RW derivedfrom DRG coding based on discharge abstract data does notreflect patient’s severity of illness accurately.32-34 Regardlessof severity of illness consideration, both hospitals andinsurance companies may be at risk of medical negligence andliability. Moreover, one factor that has not been widely usedat the stage of insurance claim is whether admitted casesencounter a complication. Although both practitioners andpayers know that a complication could be identified laterduring admission either with clinical signs or with laboratorytests, different viewpoints are often from different datareceived. In this study we found 210 out of 1,558 (13.5%,95%CI from 12.9% to 14.1%). Interestingly, 151 (72%) ofthese 210 cases were labeled as simple disease cases. The issueof severity of illness and complications should be attended tomore carefully by both practitioners and payers.
In addition, preauthorization for non-emergencyhospitalization should be taken into account to help to reduceinappropriate resource utilization from unnecessary admission.As it imposes documentation requirements and administrativeburden and may delayed necessary treatment, an effectivehealth management information system and interoperability between hospitals and payers, such as an automated utilizationreview process and electronic claim processing should beseriously taken into consideration by both parties.28 A set ofstructural data and clinical guidelines should be formulatedand agreed upon by both parties. This would standardizeroutine practice for smoother operations so resources could beallocated to improve efficiency of the whole system. Thecurrent insurance policies and provider payment methodsshould also be redesigned to create effective incentives forpatients to utilize healthcare appropriately and for hospitals toprovide medically necessary and high-quality healthcare.29-31Insurance policy holders should be well educated regardingtheir insurance coverage and exclusion.
This study suffers from some degree of incompleteinformation on severity in particular complications amongsimple disease cases. This could lead to a lowering of theestimates of RW among simple disease cases, thus compromisingthe RW. As a result, the cut-off point of 0.4 could serve as thelower possible value to differentiate simple from non-simpledisease cases. We therefore suggest setting up a registrysystem to prospectively collect data from a portion of admittedcases (10% - 30%) that are classified as simple and not simplediseases and use these data to adjust the cut-off point ifrequired.
Using 2017 anonymized data of both claimed andunclaimed cases admitted to a number of BDMS networkhospitals, we found that the RW of 0.4 could well differentiatesimple disease from not simple disease cases defined byinsurance partners. This level of RW was associated with alow proportion of complications (44/1143, i.e. 3.9%, Figure5). As a result, the RW of 0.4 could serve well to classifysimple from not simple disease cases.
Scenario analysis among 1,558 closed chart review casesshowed that increasing the RW cut-off point thresholds from0.3 to 0.4 would increase number of potential RM cases from8 to 44 cases (5.5 times) and from 0.4 to 0.8 from 44 to 165cases (3.8 times). It is obvious that while increasing thresholdbrings some benefit of detecting more Simple Disease cases,it also brings along more risks.
Different levels of percentages of simple diseases shouldbe assigned for the monitoring of hospital performance, at leastin the BDMS network. We found consistency between groupsof specific median proportion of simple diseases and medianproportion of cases below RW = 0.4, which reflects the valueof using this RW to identify simple diseases. With this tool,hospital performance could be better monitored on theirpercentage of simple diseases admitted, whether they areperforming well (in the green zone) or not (in the red zone).Those in between are in yellow zones. From our data, wepropose “Yellow zones” of 10%-20% for super tertiary care(CMI > 2.0), 40% - 50% for hub tertiary care (CMI 1.00 – 1.99),60% - 70% for basic tertiary care (CMI 0.50 – 0.99) and 70%- 80% for secondary care (CMI < 0.5) hospitals. Once theproportion of simple disease (identified using RW = 0.4) staysbelow these yellow zones, only continuous monitoring isrequired. However, when the proportion falls into the yellowzones, specific attention should be paid by hospital management.If the situation progresses and the proportion moves to higherthan the upper limit of the relevant yellow zone, specialinterventions of hospital management and insurance partnerswill be urgently needed.
We express our deep appreciation to Dr. Trin Charumilind,Chief of Doctors, BDMS for his kind suggestions and reviewof the draft manuscript. We thank Dr. Monsan Ussawanoppakiat,Insurance and Product Development Director, BDMS forproviding technical advices. Staff of Utilization Managementand Third-party-payer Services, Bangkok Hospital Headquarters(BHQ) along with Bangkok Health Research Center (BHRC),BDMS, supported data and graphical illustrations. We thankall of them for these.