Diabetes mellitus (DM) is a chronic disease that affects millions of people around the world. Management of DM requires comprehensive and ongoing care. To achieve the goal of diabetes care, the patient needs both input from their healthcare provider and their own life style modification. An appropriate patient’s behavior and self-management of DM is one of the main keys of success. DM education is a very important part of DM care and usually the outcome is better if the patient is compliant to the educator’s recommendation. The American association of Diabetes Educator (AADE)1 has defined the areas to assess and evaluate the effectiveness of the education on diabetes self-management of each individual. This involves seven self-care behaviors which include: being active (exercise), healthy eating, taking medicine, monitoring blood sugar, problem-solving especially for blood glucose, reducing risk of diabetes complications, and psychosocial adaptation.
Several studies have shown that few patients follow multiple self-care behaviors at the recommenced levels.2 Therefore, an educational program is considered to be essential in controlling diabetes or reaching a good glycemic control.Many studies found that a DM education program can increase not only knowledge but also self-management to achieve target glycemic control.3-5 The Diabetes, Thyroid and Endocrine center at Bangkok Hospital has developed a DM education pathway in order to serve as a guideline to ensure the same high quality standard of diabetes care is offered to all patients. This pathway also includes patients’ multidisciplinary visits. In the pathway, other than seeing only the doctor, the patient will also see a DM educator, a dietician and a pharmacist. This pathway helps to encourage patients to do their part to control their blood sugar, which means to follow recommended self-care behavior modification at home. The aim of this study was to evaluate the effects of the diabetes education pathway in glycemic control repre- sented by a decrease in HbA1c levels among people with diabetes exposed to this pathway.
The study was a retrospective study to evaluate glycemic control of diabetes patients who participated in a DM education pathway at the Diabetes, Thyroid and Endocrine Center, Bangkok Hospital from January, 2012 to December, 2013. The DM education pathway is delivered over 12 months for diabetes self-management instructed by a multidisciplinary team on different topics or problems at each visit for 12 months (Figure 1). All subjects involved in this pathway were interviewed by the nurse coordinator about performing exercise and self-monitoring blood glucose (SBMG). In addition, pharmacists interviewed the patients on compliance issues with drug related problems (DRP) including: 1) taking too little medication, 2) take too much medication, 3) difficulty using the dosage form, and 4) other common compliance problems associated with drug use which are frequently found in patients with type 2 diabetes mellitus.
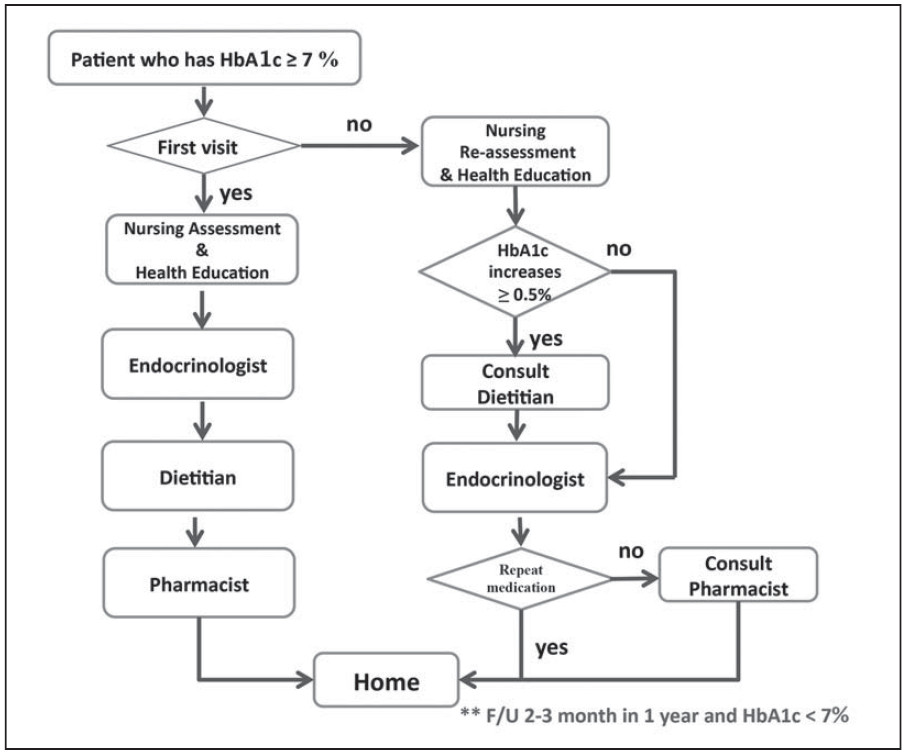
Figure 1: Type 2 Diabetic Mellitus Education Pathway.
The inclusion criteria for participants were: 1) those who had been diagnosed with type 2 diabetes, 2) aged between 15 and 80 years old and, 3) with a level of HbA1c≥ 7%. The exclusion criteria were patients who had been diagnosed with stage 4 cancer, end stage renal disease or severe medical problems or bedridden condition.
Data collected from electronic medical record (EMR) included: 1) Demographic data including age and gender,2) data of self-care behaviors including exercise behavior, self-monitoring blood glucose and drug related problems (DRP) and, 3) HbA1c level at before and after participating in the education pathways.
Data collection started after receiving approval form the Institutional Review Board and Ethics Committee at Bangkok Hospital. The data used questionnaires and data record forms from the electronic medical records to include: general information, eating habits, drug use, exercise, SMBG, and levels of HbA1c.
Statistical analysis
A descriptive analysis was used to analyze the number, percentage, mean and standard deviation of demographic data. A chi Square test was used to analyze the categorical data and a pair t-test was utilized to analyze the continuous data to compare HbA1c between before and after participating in the education pathway and the relation between the factors and HbA1c was analyzed by odds ratio (OR) with a 95% confidence interval (95% CI) and logistic regression.
Of the 163 diabetic patients participating in the study, the majority of participants were male (64.4%). The average age was 53.7 ± 11.5 years. The average HbA1c decreasedfrom 9.6 ± 2.0% to 7.6 ± 1.6% after participating in the DM education pathway for one year (p < 0.01). For behavior modification, when it came to exercise, it was found that the number of participants who performed exercise increased from 33.1% to 52.2% and participants who performed SMBG increased from 41.7% to 66.9% after participating in the education pathway for one year (Table 1).
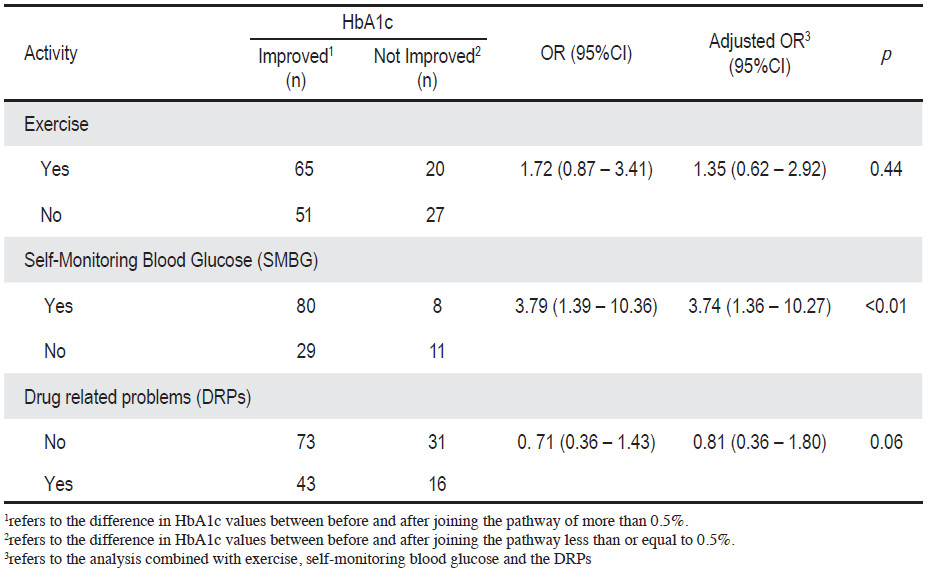
When the related factors were analyzed to find out the relationship with HbA1c after participating in the education pathway, it was revealed that using a SMBG device was associated with a decrease in HbA1c which was statistically significant (p < 0.01). For other factors including exercise, although there was no statistical relation, the patients who did exercise had lower HbA1c levels than those who did not exercise (Table 2).
Table 1: Changes in mean HbA1c, exercise behavior and Self-Monitoring Blood Glucose before and after participating the education pathway (n=163).
Table 2: The relation of the decrease in HbA1c after participating in the pathway (n = 163)
The present study aimed to assess the effect of DM education pathway in controlling HbA1c levels among adults with type 2 diabetes. The primary outcome of the study is improved glycemic levels (in terms of reduced HbA HbA1c) of patients after participating in the education pathway. The study results showed a significant decrease in HbA1c levels in participants by the end of the program (from 9.6 ± 2.0% at before to 7.6 ± 1.6% after participating in the pathway). It showed the patients who participated in the education pathway can improve their self-care behaviors and can help patients to control their blood glucose. The findings of this study are similar with the results from a previous study by Keeratiyutawong6 that showed a significant decrease in HbA1c levels in the intervention group after attending the program.
In addition, the results demonstrated that a number of patients who performed SMBG regularly showed significant improvement of levels of HbA1c. The findings of this study are similar to the results from previous studies7-12 Therefore, SMBG can help diabetic patients to control their blood glucose level and can be used as a tool to learn appropriate self-care behaviors in line with recommendation guidelines.13 However, although there was no statistically significant difference in the number of participants who showed an improvement in HbA1c levels among those who performed exercise regularly and who did not have drug related problems, it was found that the exercise increased (from 33% to 52%) and drug related problems decreased after participating in the education pathway for one year.
It is acknowledged that improvements in HbA1c levels in diabetes patients cannot be attributed solely to par- ticipating in the DM education pathway. However, the education pathway may have helped people with diabetes and multi-disciplinary team members to guide and focus on the recommended topics relating to diabetes and this tended to have a good effect on self-care behavior and glycemic control.
This study found that SMBG allowed the patients with diabetes mellitus to be able to better control their blood glucose level. The research team will share these results with diabetes mellitus patients and encourage them to perform SMBG to help them to adjust their eating habits and to exercise appropriately.
We are deeply grateful to the Bangkok Health Research Center at Bangkok Hospital and our research consultant, for their assistance in data analysis.