Ureteral obstruction is caused by several conditions. Benign causes are more common than malignant ones, and bladder and kidney stones and prostate hyperplasia occur in the majority of cases. The most common malignant causes are cervical cancer, bladder cancer, uterine cancer and colon cancer. External compression or extrinsic causes include retroperitoneal fibrosis and post radiation complications.
Surgical treatment is the modality of choice for most conditions. Occasionally, conservative treatments of either endoscopic or percutaneous interventions are considered. Retrograde DJS is more commonly used than percutaneous nephrostomy (PCN). Studies have not shown any clinical advantages of DJS over PCN in terms of safety rates (major complications)1 or comfort (quality of life scoring).2 That said, most patients and physicians continue to favor DJS over PCN.
Plastic-based materials in DJS and nephrostomy tubes are either made of silicone, polyethylene and/or polyurethane but the latter proves to be the most durable. The median durability of both DJS and PCN is less than 6 months. Causes of a non-functioning stent stem from either encrustation or obstruction that may be connected to bacteriuria that may in turn lead to septicemia or sepsis which is the most serious complication. Biofilm occurred in 60-90% of cases leading to bacteriuria in 30%. E.coli and enterococcus are found in 44% of all colonizations.3 Normally, there are three (3) stages in developing biofilm: 1) endogenous protein deposition; 2) bacterial attachment and; 3) development of biofilm structure. In any case, tumor ingrowth or over-growth are mechanisms of obstruction in most malignancies. Other major complications besides infection range from hematuria, bladder spasm, dysuria and flank pain. Most guidelines recommend a stent exchange every three (3) to six (6) months.
The tubed- or self-expandable metallic stent has been reported in cases of ureteral obstruction for more than a decade such as the WALL stent, Nitinol stent or other newly developed metallic stents. Stent migration is still the major problem in 30% of cases. 4
In 2007, the Resonance® stent (COOK Medical, Bloomington, IN) was introduced. A full length double-J stent constructed of a spirally coiled nickel-cobalt-chromiummolybdenum (Figure 1) was approved by US FDA for use in ureteral obstruction. The Resonance® stent has an advertised in situ lifespan of 12 months and higher radial strength, in theory increasing resistance to external compression, decreasing cost/morbidity of stent changes, and the need for PCN. Initial results were uniformly positive, with early data indicating stents could maintain good functionality with minimal encrustation despite lengthy periods of time in situ. The write-up information claimed a 12 months interval. Most previous reports were performed with a retrograde approach using endoscopic assistance.
We have experience of four (4) cases using Resonance® stent performed in antegrade approach via a percutaneous nephrostomy. We report and discuss in detail one reported case
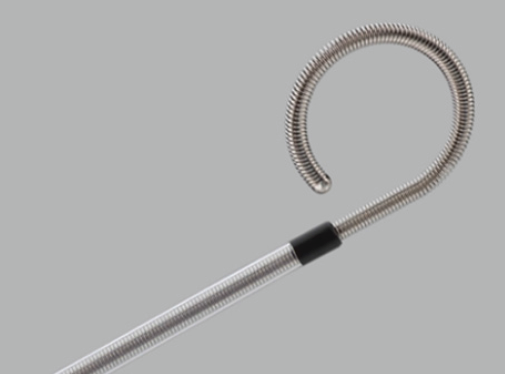
Figure 1: Shows photo of Resonance® stent. A full length double-J stent constructed of spirally coiled nickel-cobalt chromiummolybdenum.
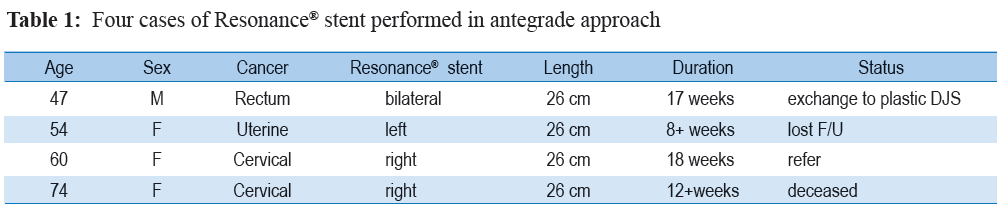
A 74-year old Arabic female presented with diagnosed cervical cancer with a history of external radiation for 20 years. The disease was recurrent a few years ago and palliative external radiation was performed. Recently, the disease developed to an advanced stage and the patient developed bilateral obstructive uropathies due to a urinary bladder invasion. Patient was given bilateral PCN and there was existing left plastic DJS performed in the home country. Patient manifested with seizures due to brain metastasis and presented with sepsis on the day of admission.
Ultrasonography of KUB system revealed a moderate degree of hydronephrosis on the right kidney and minimal dilatation of pelvocalceal system on the left kidney. An interventional radiologist was consulted to revise the PCNs and DJS. Fistulography was done on both kidneys via the PCNs and a right ureterovesicle (UVJ) obstruction was found with a still functioning left DJS which was confirmed by the passage of contrast media from the kidney through the ureter into the bladder (Figures 2-4).
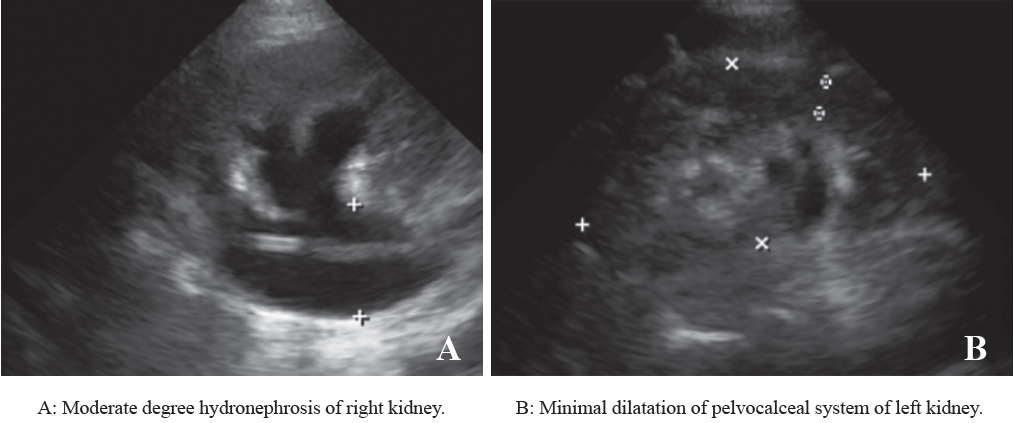
Figure 2A-B: Ultrasonography
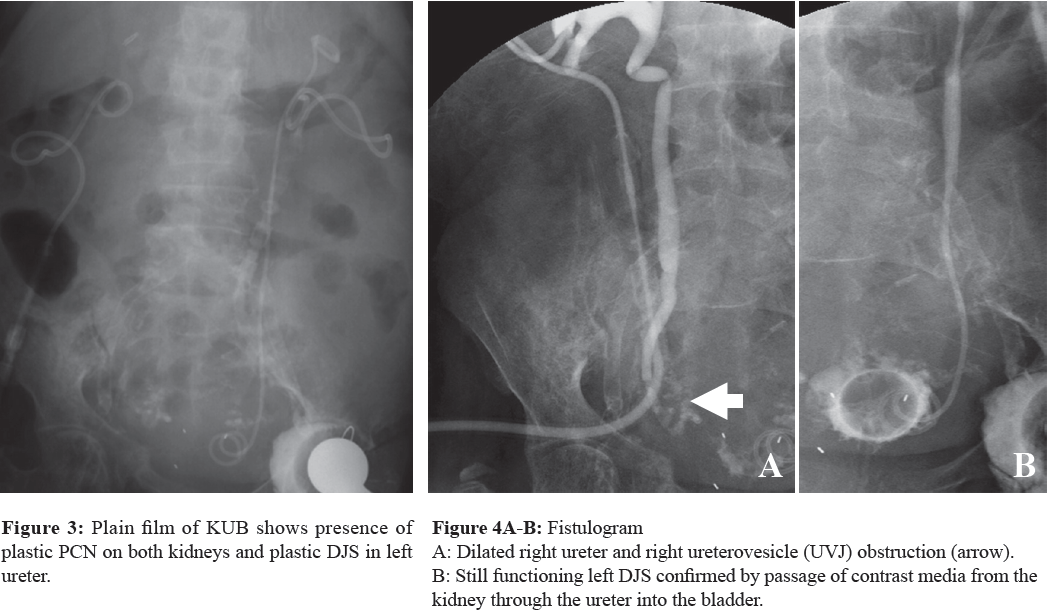
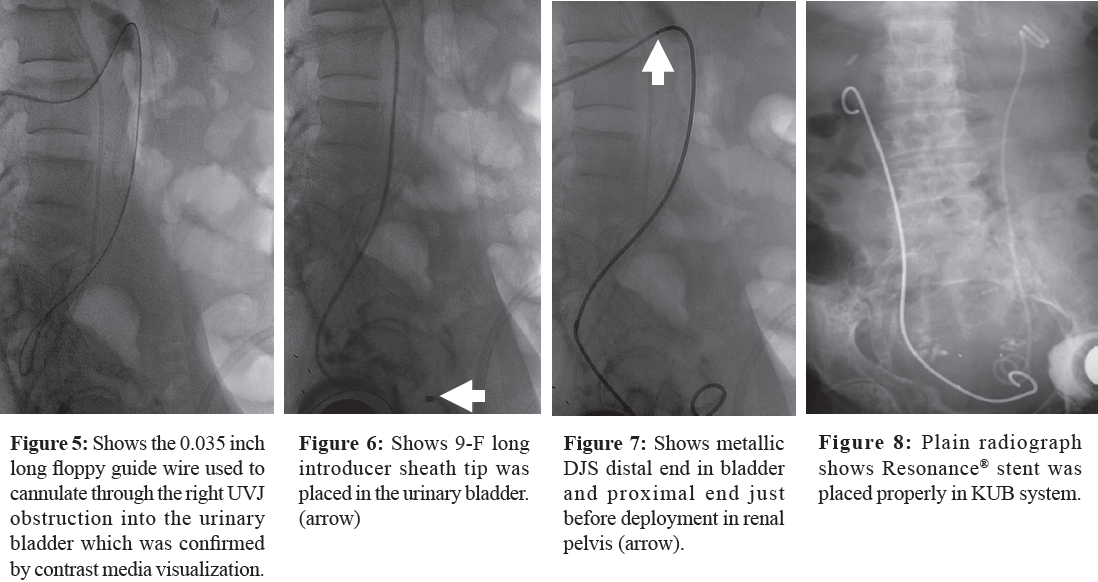
Left PCN was removed after confirming well-functioning left DJS. It was decided to correct the Right UVJ obstruction with an antegrade approach of DJS. The old Right PCN was cut and removed after placing a 0.035 inches long floppy guide wire and a vascular introducer sheath of 9.0- F was placed under fluoroscopy. Assistance of a 5-F diagnostic Cobra catheter and a 0.035 inches long floppy guide were both used to cannulate through the right UVJ obstruction into the urinary bladder which was confirmed by contrast media visualization (Figure 5). An exchange of the floppy guide wire of 0.035 inches was made with a 190 cm long stiff Amplatz guide wire and then the diagnostic catheter with 9-F introducer long sheath was replaced, (this was provided in the Resonance® stent kit set). The 9-F long introducer sheath was inserted via the vascular introducer sheath 9-F (placed in the right renal pelvis) and its tip was placed in the urinary bladder (Figure 6). The 6-F, 26cm long Resonance® stent was inserted into the introducer sheath and pushed in an antegrade fashion with the assistance of a pusher catheter until the distal end of the DJ metallic stent presented in the urinary bladder under fluoroscopy. Selection of stent length and adjustment of stent position were determined by patient height and ureter length. Most parts of the distal end of the stent tended to be placed in the urinary bladder and we were concerned with the positioning of the proximal end of the DJS which was rather difficult to place accurately in the right renal pelvis (Figure 7). A careless deployment of the proximal end of DJS that had been placed with an antegrade approach may have led to the malpositioning of the stent in kidney parenchyma. After deployment of the DJS, the fistulogram was checked with injection of contrast media through the already placed 9-F vascular sheath. Once
the proper position of the metallic DJS was confirmed as there was no visualization of contrast leakage in either the kidney parenchyma and retroperitoneum, the 9-F vascular sheath was then removed (Figure 8). Manual pressure for 2 minutes was performed. Bleeding and urine leakage were checked. Patient was sent to the recovery room. The procedure time was 30 minutes and the patient was given moderate sedation by the anesthesiologist. Patient vital signs were stable with no presence of hematuria postoperative. Patient was alive with metallic stent 3 months following and died due to progression of disease in the brain.
Patel et al. 5 reported 12 months median indwelling time of Resonance® stent in the malignant ureteral obstruction group and 19 months in the non-malignant group of a 52 cases series. But most of the retrospective and prospective studies between the years of 2013 to 2016 report a median duration of 5-12 months. Technical success rates of the retrograde endoscopic approach were about 90%. There were no serious complications reported. The most common complications reported are hematuria (7-15%), UTI require removal of stent (6-12%), migration (1-20%) and irritative voiding symptoms (8-19%).6-12
The mechanism of stent occlusion in the Resonance® stent is very different from the plastic stent. Although the macroscopic appearance appears clean it is actually covered by a thin layer of encrustation and its surface is observed by electron microscopy showing a high concentration of calcium and phosphate deposits in energy dispersive analysis.13
Cost analysis and quality of life studies14 conclude that the Resonance® stent is well tolerated by patients with ureteral obstruction of various etiologies and it provides a significant financial benefit compared with polymer ureteral stents. For patients who are not fit for surgical intervention regarding their ureteral occlusive disease, the metal Resonance® stent is a financially advantageous and well-tolerated option.
Uthappa and Cowan in 200515 compared retrograde vs antegrade approach of plastic DJS placement in 50 patients. Technical success was 96% in antegrade or percutaneous approach compared to 50% in endoscopic retrograde approach. They suggested that the retrograde route should be the initial approach if imaging shows no involvement of ureteric orifice (UO), when nephrostomy is technically very difficult or in cases of a solitary kidney. The antegrade route is preferred if imaging shows tumour occlusion of the UO or if there is a tight stricture very close to the uretero- vesical junction (UVJ) making purchase within the ureter difficult for crossing the stricture. There were limited reports of Resonance® metallic stent placement via the antegrade route or percutaneous approach.15-17 The results did not show any difference in the success rate, patency and incidence of complications compared to the retrograde or endoscopic approach.
Our experience using the Resonance® stent is limited. That said, we found that the technique to place this metallic stent on an antegrade basis was not unduly complicated. A very short learning curve to perfect this skill is needed and there are very few potential pitfalls. An operator who is used to working with other kinds of stent deployment will understand and follow the Resonance® deployment technique easily. If we can catheterize through the ureteral obstruction and reach the urinary bladder, the next step is not that difficult. The only technical disadvantage is its larger access that requires the 9-F access system. This may lead to bleeding complications compared to the smaller access required in the case of a plastic DJS.
As the cases studied are limited, we could not reliably conclude how long the patency is and how often complications may occur. There was early obstruction in one (1) of the cases but the follow up with the rest of the cases was not possible.
The retrograde or endoscopic approach of DJS is still the most favorable choice of treatment in both benign and malignant ureteral obstructions. PCN is a viable alternative to DJS placement. Antegrade placement of DJS, either plastic or metallic, can be done easily with no significant complications particularly when the PCN tube is already placed in the kidney. Metallic DJS or Resonance® stent is probably advantageous to plastic DJS in terms of median durability and cost effectiveness. We recommend the use of the metallic DJS or Resonance® stent in patients with failed placement of DJS with retrograde or endoscopic route and patients who have an encrusted PCN catheter.
The authors claim no conflict of interest associated with the manuscript