DNA mismatch repair (MMR) is necessary for all organisms in order to maintain DNA integrity. Loss of expression of one of the MMR proteins results in several sporadic and inherited human cancers of various organs such as colon, rectum, stomach, uterus, and ovary.1 Microsatellite instability (MSI) was shown to be associated with some cancer types, better survival and/or outcome, and reduced likelihood of distant metastases and susceptible to chemotherapy.2-4 Either immunohistochemical study showing loss of MMR proteins expression or PCR-based assay for microsatellite instability can be used to evaluate the MMR status of cancer tissue.5
Colorectal cancer (CRC), particularly those occurring in the setting of Lynch syndrome, is the prototype of malignancy with microsatellite instability. MMR status has extensively been studied in CRCs3,4,6-10 and although deficiency of DNA mismatch repair was reported in 15% of Thai patients with sporadic CRCs,11 MSI testing is not routinely performed as part of the clinical practice in Thailand.
Immunotherapy has played a significant role in cancer treatment and recent clinical studies have suggested that mismatch repair–deficient cancers, regardless of tissue origin, are susceptible to immune-checkpoint inhibitors e.g. PD-1 blockade.12,13 In May 2017, the US Food and Drug Administration (FDA) granted an accelerated approval to pembrolizumab, an antibody to the PD-1 receptor, as an alternative treatment for unresectable or metastatic MSI-H and MMRdeficient solid tumors. This was the first approved drug merely based on biomarker status, not the location or extent of cancers.14 The purpose of this article is to report of our recent experience with MSI testing.
Study Population
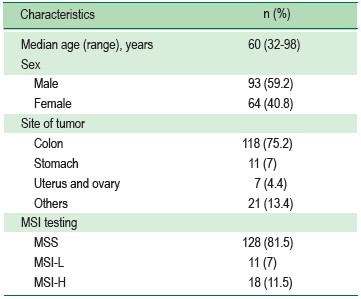
A total of 157 Thai patients from King Chulalongkorn Memorial Hospital and other hospitals (all private hospitals) underwent microsatellite instability testing at Chulalongkorn GenePRO Center, Faculty of Medicine, Chulalongkorn University between July 2013 and July 2017 were enrolled in this descriptive retrospective study. All diagnoses were pathologically confirmed. This study was approved by the Institutional Review Board, Faculty of Medicine, Chulalongkorn University (COA No. 292/2018 and IRB No. 107/61). Patient characteristics are summarized in Table 1.
Microsatellite Instability (MSI) Testing
Normal and tumor genomic DNA were extracted from whole blood and formalin-fixed paraffin embedded (FFPE) tissue using QIAamp® DNA blood mini kit and QIAamp® DNA FFPE Tissue Kit and (Qiagen), respectively. The amount and quality of DNA were measured at absorbance 260 nm and 280 nm using nanoDropTM 2000 Spectrophotometer (Thermo Fisher Scientific). Matched normal and tumor DNA were investigated with a set of 5 microsatellite markers including BAT25, BAT26, D2S132, D5S346 and D17S250.15
PCR amplifications were performed with 60 ng of purified genomic DNA using VeritiTM Thermal Cycler (Applied Biosystems). Each PCR admixture had 20 uL of volume containing 1X Gold buffer, 1.5 mM MgCl2, 200 μM dNTP, 0.2 μM of each primer, 1.25 unit AmpliTaq® gold DNA polymerase (Applied Biosystems). The PCR amplification was performed using a condition as follows: initial denaturation at 95°C for 10 min followed by 45 cycles of 95°C for 30 sec, 55°C for 1 min, and 72°C for 1 min and then final extension at 72°C for 5 min. The PCR products were subsequently visualized using 8% polyacrylamide gel electrophoresis stained with SYBR® DNA gel stain (Invitrogen) and Gel DocTM XR+ Gel Documentation system (BioRad). For fragment analysis, 1 μL of 10-fold dilution of PCR products was mixed with 8.7 μL Hi-DiTM formamide and 0.3 GeneScan™ 500 LIZ® Size Standard (Applied Biosystems) and incubated at 95OC for 5 min. Then, PCR fragments were detected using 3130 Genetic Analyzer (Applied Biosystems). The results were subsequently analyzed using GeneMapper® Software Version 4.0 (Applied Biosystems).
Table 1: Characteristics of patients related to the samples used in this study (n = 157)
High microsatellite instability (MSI-H) and low microsatellite instability (MSI-L) were, respectively, defined as ≥ 2 and 1 of the 5 loci examined showing different microsatellite pattern(s) between normal and tumor tissue.6,15 Microsatellite stability (MSS) was designated when all 5 loci show no different pattern between normal and tumor tissue.
At Chulalongkorn GenePRO Center, we started MSI testing in 2013 but received only a few cases per month. In 2015, there was a dramatic increase in the number of cases submitting to our lab for the assay (Figure 1), and this trend was more pronounced in private hospitals compared to the King Chulalongkorn Memorial Hospital.
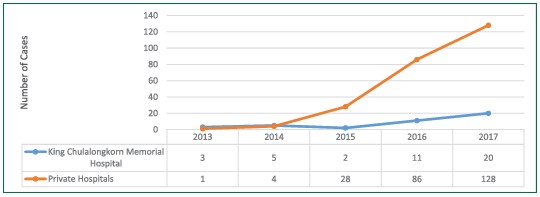
Figure 1: Trend of MSI testing at King Chulalongkorn Memorial Hospital and private hospitals.
Among 157 tumors from the study population; MSI-H, MSI-L, and microsatellite stable (MSS) tumors were detected in 18 (11.5%), 11 (7%), and 128 (81.5%) patients, respectively. Out of the 18 MSI-H cancers; 13 (72.2%), 4 (22.2%), and 1 (5.6%) were colorectal carcinoma, gastric carcinoma, and carcinosarcoma of uterus and ovary, respectively. Representative chromatograms showing MSI-H cancer are displayed in Figure 2. Frequency of cancer locations in MSI-L and MSI-H subgroups are described in Table 2; and details on the instability rate for each microsatellite marker in Table 3. BAT25 and BAT26 markers were universally unstable in all MSI-H tumors.
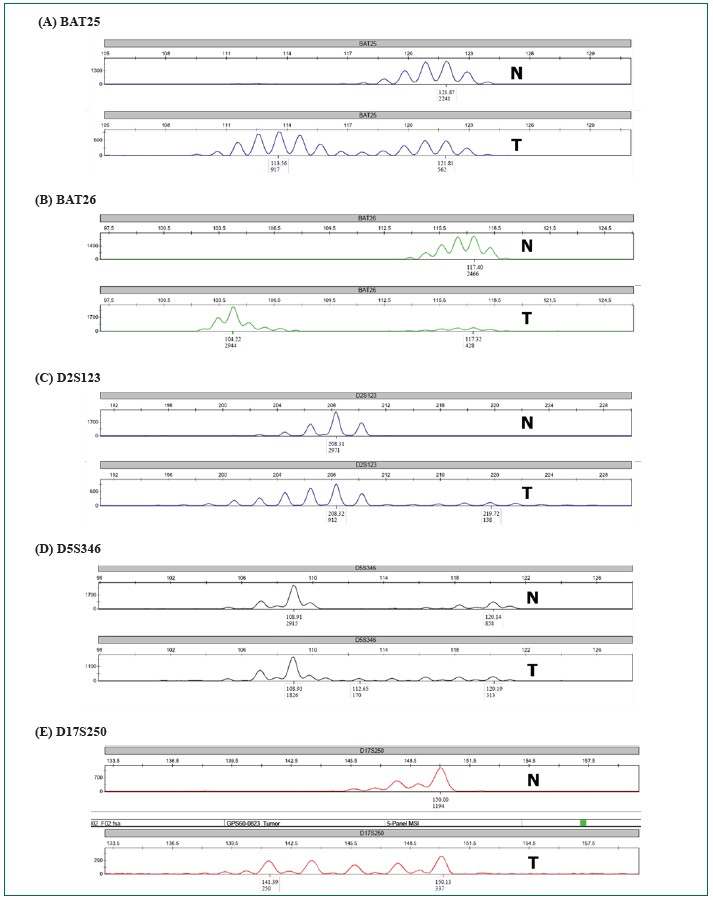
Figure 2: Representative fragment analysis of 5 microsatellite loci are shown (A-E), all demonstrating microsatellite instability (N = normal DNA, and T = tumor DNA).
Table 2: Frequency of cancer locations in MSI-L and MSI-H subgroups
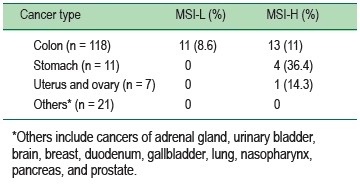
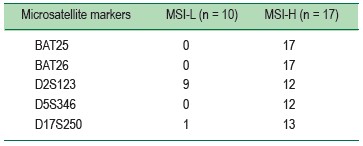
Table 3: Instability of each microsatellite marker in 10 MSI-L and 17 MSI-H tumors
Although cancers are well-known to develop through multiple genetic/epigenetic abnormalities, molecular tests in cancers in Thailand are typically driven by drugs. For example, testing for RAS mutation in CRCs in Thailand was started only when there was a need to give EGFR monoclonal antibody to advanced cases. The situation holds true for the MSI testing in CRCs that was rarely requested by the clinicians before the year 2015. In that year, a small phase 2 clinical trial (n = 41) demonstrated that pembrolizumab, an anti-PD-1 antibody, benefited patients with mismatch repair-deficient (MMR-D) solid cancers, regardless of the primary site.16 Since then, requests for MSI testing have significantly increased at our center, especially from the private hospitals (see Figure 1). Even though our study is limited due to the lack of clinical data, it is tempting to speculate that the increasing demand for MSI testing is associated with the study mentioned above.
In 2017, a larger series of MMR-D solid cancers was shown to be sensitive to PD-1 blockade.12 A total of 86 patients with MMR-D tumors of various organs were recruited, including 40 (47%) colorectal, 15 (17%) endometrial, 8 (9%) pancreatic, 5 (6%) gastroesophageal, 5 (6%) small bowel cancers, and others (cancers of ampulla of Vater, bile duct, prostate and thyroid). There were 39 (45%) patients with detectable germline mutation (Lynch syndrome). Objective radiographic responses were observed in 53% (46/86 patients), with 8 patients (21%) showing a complete radiographic response. Disease control (partial response and complete response and stable disease) was achieved in 66 patients (77%). The distribution of primary site of MMR-D cancers enrolled in the study is rather similar to our cohort in which colorectal and gastric cancers showed high prevalence of MSI-H. The overall prevalence of MSI-H CRCs in our patients (11%, n=118) is slightly lower than that (15%, n= 211) reported in Thai population by Korphaisarn et al.11 Varied study populations and sample size may have resulted in the differences. While the previous Thai series included all stages of CRCs, all of our patients are presumably advanced stage and MSI testing was likely requested for immunotherapy. The high frequency of MSI-H noted in 4/11 (36.4%) gastric cancers is of interest but this should be further confirmed by a larger series.
According to National Cancer Institute (NCI) guidelines, the recommended microsatellite panel for MSI testing comprises of 2 mononucleotide repeats (BAT25 and BAT26) and 3 dinucleotide repeats (D2S123, D5S346 and D17S250). MSI-H tumors are defined as those with instability observed in two or more microsatellite markers whereas only one marker is unstable in MSI-L tumors.6,15 The 5 markers were also used in our center, and it is of note that both BAT25 and BAT26 were unstable in all MSI-H tumors in our present cohort, similar to the previous studies.7-9 Therefore, care should be taken before scoring a MSI-H tumor with stable BAT25 or BAT26; samples mix-up must be first excluded. Given the high frequency of BAT26-unstable tumors, one study suggested that BAT26 may be used for the initial MSI screening in sporadic CRCs in regions with limited resources.10 We do not agree, however, with this suggestion since it may complicate the laboratory workflow, delay the turn-around time, and may not save much in term of costs.
Immunohistochemical (IHC) study for mismatch-repair proteins is an alternative approach to identify MMR-D cancers in places with no access to MSI testing. MLH1, PMS2, MSH2, and MSH6 are most commonly tested by IHC. Both approaches complement each other. While normal tissue or blood of the particular patient is needed to perform MSI testing, IHC can be run without significant amount of normal tissue.
We have experienced a dramatic increase in MSI testing in our center. Colorectal cancers were most frequently tested, and accounted for the highest percentage among MSI-H tumors. The high frequency of MSI-H observed in 4/11 (36.4%) gastric cancers is of interest but this figure should be further assessed by a larger series.
This study was partly supported by the National Research Council of Thailand Grant under the Research University Network (RUN) Initiative.